The Center for Advanced Imaging at NorthShore University HealthSystem (NorthShore) combines clinical expertise with innovative developmental research. This combination promotes continuing advances in our clinical services and drives research efforts towards clinical relevance. The breadth of expertise of our group provides a rich and stimulating environment. The group is actively engaged in enhancing the diagnostic value of MR imaging through the pursuit of fast imaging approaches, 3D volumetric imaging techniques and physiologic imaging. Physiologic imaging complements the traditional anatomic imaging and is anticipated to expand services that will favorably impact patient care.
Dedicated whole body research systems at 1.5 Tesla and 3.0 Tesla allow for rapid development of new approaches for Magnetic Resonance Imaging (MRI). The program clearly benefits from the strong collaborations with world-renowned clinicians, basic and clinical scientists. These studies are still in the research phase and are not yet used as clinical exams. Our current interests and expertise include, but is not limited to:
MR Angiography and Venography Throughout the Body
At present, the clinical standard for detection and staging of structural abnormalities of the aorta and its branches is x-ray arteriography. For the most part, x-ray arteriography is well tolerated but is not without risk. Bleeding and vessel trauma from the introduction of the catheter into the vascular system, allergic reactions to the iodinated contrast in certain individuals as well as renal failure due to dye toxicity are some of the risks, as well as ionizing radiation. Magnetic Resonance Angiography (MRA), introduced in mid 1980s continues to make rapid progress with newer and better imaging techniques to detect and evaluate abnormalities of the aorta and its branches. Without introducing a catheter into an artery or exposing the patient to either potentially toxic dyes or radiation, MRA provides physicians with increasingly more accurate pictures for diagnosis and assessment in a variety of disease processes. Currently, we are looking at MRA applications to legs and feet, to the body and to imaging the coronary arteries. Each has their own special needs and limitations. We are trying to push the technological limits to provide robust angiographic images that can be routinely used in the clinic.
MR Evaluation of the Vascular System
The thrust of our research is to use and to develop magnetic resonance imaging technologies to evaluate the vascular system. A specific area of investigation is the use of MRI to non-invasively study atherosclerosis, a systemic vascular disease also referred to as ‘hardening of the arteries’ that causes ailments such as heart attacks and strokes and ultimately is the leading cause of death in the United States. The overriding goal of this research is to develop MR methods that are capable of identifying high-risk atherosclerotic lesions and that can be used to guide medical or pharmacological therapy. Another area of interest to our group is the development of new MRI technologies for angiography that do not require contrast material to be injected into the blood stream. With further development, these contrast-free exams may eventually replace more invasive diagnostic tests that expose patients to more risk and discomfort.
Non-Invasive Imaging
Imaging technologies are being tested that offer new ways to see inside the human body that yield unprecedented image quality without the need for invasive procedures like intravenous or intra-arterial catheterization. These rely on the fact that blood has distinctive physical properties compared to background tissue such as fat and muscle, and do not depend on blood flow for clear resonance. As diagnostic tools these offer new “platform technologies” which draw many converging disciplines. The procedures will have a major impact on multiple specialties and physicians, including radiologists, vascular surgeons, cardiologists and neurologists. The most immediate application is the diagnosis of peripheral vascular disease.
Development with Industry – Clinical Trials
MRI has evolved with faster sequences, functional imaging and multi-channel technology. We are in a clinical trail designed to test the safety and efficacy of a new contrast agent that may be better suited for these changes. We are also testing a new contrast agent to evaluate renal veins and arteries without the use of radiation as is currently needed for digital subtraction angiography, a common clinical test.
Magnetic Resonance Imaging of Stroke
Early intervention is critical if one is to salvage brain tissue injured during a stroke. We have developed a method, based on magnetic resonance diffusion imaging, for very early detection of the region of stroke. This technique is currently being used to assist doctors in more accurate early diagnosis, and to monitor the effectiveness of various therapeutic interventions.

Brain areas active when studying faces are shown. Visual areas appear bright orange and yellow at the back of the brain (shown here at the right of the figure), whereas memory areas involved in learning to recognize the faces appear red within the cutaway section.
|

This cutaway picture of the brain illustrates areas more involved in learning to recognize faces (red) and those more involved in remembering faces (green).
|
3D and Functional Brain MRI
Using high-resolution MR and CT images in conjunction with the Center's advanced image processing facility, 3D brain maps are constructed that allow surgeons to plan neurosurgical procedures in a more effective way. These 3D maps are also valuable teaching aids, whereby a surgical trainee can perform virtual procedures on the computer screen before attempting the procedure in a patient. MRI can be used for more than just displaying anatomy; for instance, functional MRI is being applied to better understand the basis for various neurological and psychiatric disorders and the effects of therapy.
MR Evaluation of Renal Physiology & Function
It is now well recognized that the renal medulla operates at low oxygenation level (hypoxia) and this has serious implications in several disease processes. Our laboratory has pioneered in the use of Blood Oxygenation Level Dependent (BOLD) MRI to study renal oxygenation status in both small animal models and humans. The technique is now being used world-wide by different groups to study effects of different diseases and the effect of drugs. We are now working on translating our experience in rodent models and healthy human subjects to people with and at risk of Chronic Kidney Disease (CKD).
Currently, there are an estimated 15.5 million adults in the US with stage 3 and about 1 million with stage 4 or 5 CKD. About 330,000 are on dialysis and the rest (700,000) are close to initiation of renal replacement therapy including renal transplantation. A clinically pertinent question is “Who among those defined as CKD stage 3 (based on current standard of care) will really progress towards end stage renal disease (ESRD) (estimated to be only a third)?” This has led to growing interest in development of alternate biomarkers that may identify subjects at risk of progression. We believe MRI offers several markers including BOLD MRI that could potentially identify subjects at risk of progression and this is our current interest.
Prospective Investigation of Quantitative MRI in the Diagnosis of Alzheimer's Disease
We have developed a high resolution magnetization transfer (MT) technique enable us to probe the subtle changes in the brain regions that affected by Alzheimer’s Disease (AD) in the early stage. By automating the process of defining the region of interests, one will eliminate the human bias and will have significant impact on the consistency of clinical trials that use MR measurements of the hippocampus. We have initiated a prospective multidisciplinary Alzheimer’s clinical study that is designed to evaluate the utility of the new MR imaging technique for the detection of structural changes in the entorhinal cortex and in the hippocampus as early signs of AD. This study involves MDs and PhDs from six different departments at NorthShore: Radiology, Neurology, Psychiatry, Family Medicine and Geriatric Medicine.
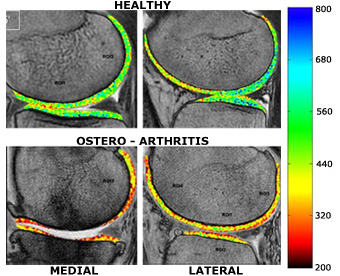
Figure shows dGEMRIC “T1” maps obtained from a representative healthy subject and a subject with documented osteo-arthritis. The colors have been chosen such a way that “diseased or degenerated” cartilage will appear more towards red while healthy cartilage would appear more towards green and blue. It is not surprising that the medial cartilage appears red with evidence of complete cartilage loss in the weight bearing region in the subject with OA, the question is “is the lateral cartilage showing signs of early disease?” “If so, can it be reversed?” These are the questions we are trying to answer.
Osteoarthritis
Osteoarthritis (OA) is an important cause of disability in our society, affecting millions and resulting in loss of time at work and activity limitations. OA is primarily a disease of articular cartilage, either from injury or from degeneration. MRI, with its excellent soft tissue contrast, is the best technique available for assessment of articular cartilage. In addition to exquisite morphological information, many tissue parameters that can be measured by MRI techniques have the potential to provide biochemical and physiological information about the cartilage and its repair. One such method is delayed gadolinium enhanced MRI of cartilage (dGEMRIC), a technique that has been shown to be sensitive to changes in glycosoaminoglycans (GAG), a constituent of articular cartilage that is known to be depleted early in the development of OA. While current treatment for OA is primarily geared towards symptom relief, new drugs are in development that would potentially modify the disease process. dGEMRIC can provide a way of early detection of OA prior to gross and irreversible anatomical changes and also allow for an objective way to follow changes with novel interventions. This technique is still in the developmental stage and not yet available for clinical use.